Rehabilitation
Rehabilitation
Outpatient Rehabilitation
What is Outpatient Rehabilitation?
This is rehabilitation conducted at our hospital while the patient continues living at home.
Our team is dedicated to providing daily care and treatment for individuals who have been discharged from acute or recovery-phase hospitals but still face uncertainties about resuming daily life, those experiencing difficulties after discharge, and those who have not been hospitalized due to illness or injury but struggle with daily activities. Our goal is to help them lead healthy and fulfilling lives at home.
Features of our outpatient rehabilitation
Orthopedic disorders
We provide rehabilitation for shoulder, knee, foot, and other joint disorders; after artificial joint replacement surgery; for spinal disorders, such as lower back pain and spinal stenosis; for shoulder periarthritis (also known as frozen shoulder); for sports injuries, such as tendon rupture; and after surgery
Cerebrovascular diseases
Sequelae of cerebral infarction and cerebral hemorrhage, sequelae of subarachnoid hemorrhage, and sequelae of cerebral embolism.
Neuromuscular diseases
Parkinson's disease, neurogenic supranuclear palsy, and spinocerebellar degeneration.
We provide rehabilitation services for various ailments tailored to the patient's physical condition upon understanding each person's disability and performing a multifaceted examination of their daily living conditions. Additionally, consultations for the repair or creation of orthotics are available within our outpatient rehabilitation services. Orthotic devices are created through collaboration between physicians, physical therapists, and prosthetists.
Free home pick-up service
Our hospital provides a home transportation service for those who receive outpatient visits (rehabilitation).
Flow of outpatient rehabilitation
During an outpatient consultation, the attending physician will discuss the need for rehabilitation.
The attending physician selects and prescribes the necessary rehabilitation from among physical therapists, occupational therapists, and speech-language pathologists based on the individual needs of the patient.
Rehabilitation staff will be available to assist. Because it is generally by appointment, please wait in the waiting area outside the consultation room.
We will confirm the initial rehabilitation appointment, availability of transportation, and rehabilitation deadlines.
After examination by the attending physician, our rehabilitation staff will pick you up. Please wait in the waiting area outside the consultation room.
We assess physical function and activities of daily living and provide individualized treatment. Additionally, we provide suggestions and guidance for exercises that can be done independently at home. The rehabilitation supervisor will propose rehabilitation goals, approximate completion date, rehabilitation time, and frequency of visits (The frequency and duration of rehabilitation will depend on the physician's orders and the patient's condition.)

The patient will be reevaluated every 3 months to reassess rehabilitation goals, time of completion, and frequency of hospital visits.
We provide guidance on important considerations for home life, along with suggestions and instructions for self-training exercises.
If there is a transferring organization, we will provide information to ensure a smooth transition.
Outpatient Rehabilitation Consultation Hours
| Mon | Tue | Wed | Thu | Fri | Sat | ||
|---|---|---|---|---|---|---|---|
| A.M. | 9:00〜12:00 (Reception until 11:30) |
○ | ○ | ○ | ○ | ○ | - |
| P.M. | 13:00〜17:00 (Reception until 16:30) |
○ | ○ | ○ | ○ | ○ | - |
〈No-consultation days〉
Saturdays, Sundays, Public holidays, Year-end and New Year holidays (December 30–January 3)
and the frequency (number of times) of implementation may be limited. For more information, please contact our rehabilitation staff.
if you have any questions.
Inpatient Rehabilitation
Individual Rehabilitation
Our physical therapists (PT), occupational therapists (OT), and speech therapists (ST) provide inpatients with individualized and comprehensive evaluations of their motor, cognitive, swallowing, and language functions, as well as other physical functions and abilities to perform daily living activities. Based on this, we create the optimal rehabilitation program, providing rehabilitation for a maximum of 2–3 hours per day, 365 days a year in our rehabilitation ward.

Physical therapy

Occupational therapy

Speech and hearing
Group Rehabilitation
We provide various recreational activities for inpatients or patients in residential care to maintain and improve their physical functions through enjoyable activities, to increase the effectiveness of dementia prevention, and to refresh their minds.

Creative recreation
Enjoy making seasonal collages, wall decorations, and accessories.

Events
Seasonal events will be held. Preparation is done together with inpatients and patients in residential care.

Oral and swallowing exercises
Before lunch, dental hygienists and speech therapists jointly conduct oral and swallowing exercises.

Occupational activity
Various occupational activities are carried out according to the patient's interests.

Horticultural therapy
We aim to promote social well-being through engagement with horticultural plants, such as flowers and vegetables.
Dysphagia therapy
What is dysphagia?
A condition in which any behavior related to “eating” is impaired in one's diet is called “dysphagia.”
Inability to eat by mouth・・・
causes dehydration and malnutrition
Decrease in swallowing function・・・
causes aspiration pneumonia and choking.
Loss of enjoyment in eating・・・
decreases motivation in life.
Characteristics of our dysphagia therapy
Under the guidance of our physicians, speech therapists, dental hygienists, nurses, and dietitians work together to provide feeding and swallowing rehabilitation.
Our goal is not to provide nutritional intake for each patient but to support a life of “enjoying food safely and securely.”
(1) Speech therapists provide swallowing evaluation and training
We evaluate the entire process, from recognizing food to taking it into the mouth, chewing, swallowing, and the sequence of actions from the throat to the esophagus. In some cases, a swallowing videofluorography is performed.
(2) The oral cavity is evaluated by a dental hygienist.
The primary evaluation involves oral function, such as evaluating whether oral hygiene is maintained and whether dentures are in place. In some cases, a dental consultation will be arranged.
(3) We provide meals suited to each patient's condition after reviewing them with speech therapists and dietitians.
The meal format is gradually upgraded from swallowing initiation diet, through swallowing training diet, to nursing care diet to implement safe oral transition.

Activities of daily living (ADL) practice
What is ADL practice?
ADL refers to Activities of Daily Living. A refers to Activity and DL refers to Daily Living (daily living). These refer to the basic daily living activities necessary for daily life, including 'transfers, mobility, eating, dressing, toileting, bathing, and grooming.'
Our hospital emphasizes early recovery of ADL activities necessary for discharge home or admission to a facility and provides support 24 hours a day as a team approach in cooperation with the rehabilitation department and other professions.
Practice in changing clothes

Practice in managing one's personal appearance
IADL
For patients who need more advanced activities of daily living to be discharged home, we actively support them in acquiring instrumental activities of daily living (IADLs).
Practice using a vacuum cleaner

Dishwashing practice

Physiotherapy
What is physiotherapy?
This refers to medical treatments that use physical forces, encompassing therapies that involve electrical currents, sound waves, heat, and cold stimuli. Each physical stimulus is intended to produce some therapeutic effect, such as excitation or inhibition of cells, tissues, nerves, or muscles, and physiotherapy is sometimes considered a part of physical therapy. In such cases, they are broadly classified into “exercise therapy,” “physiotherapy,” and “movement training” and are performed mainly in rehabilitation settings under the specific direction of a physician.
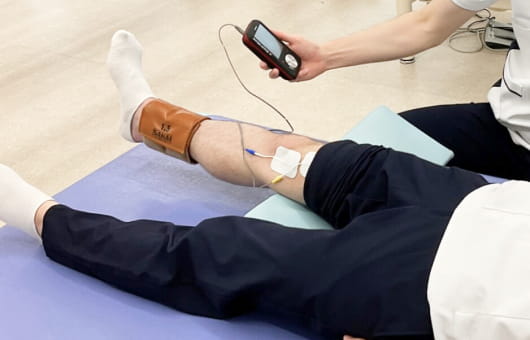
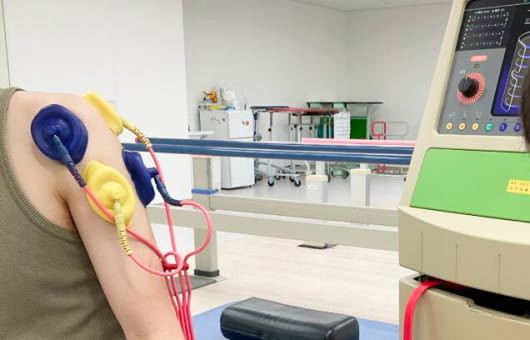
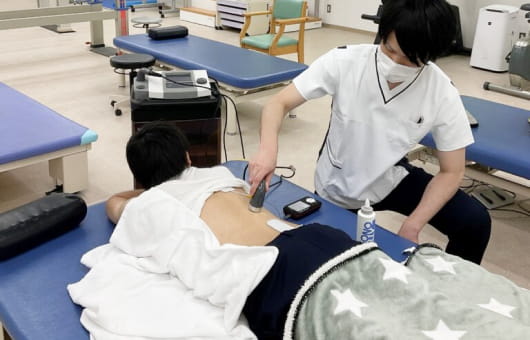
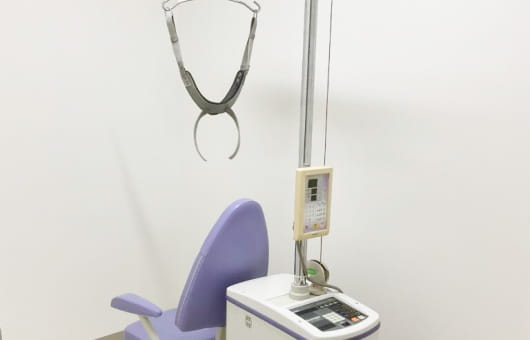
Introduction of our physiotherapy equipment
Our Approach
In recent years, these physiotherapy techniques have been rarely used alone but in combination with exercise therapy.
The American Physical Therapy Association (APTA) states that “if used in the field of physical therapy, it should be combined with other treatments such as exercise therapy, and physical therapy should not be used alone unless there is clear evidence that it is clearly more effective as a standalone treatment.”
We will provide a combined approach in consultation with the physician, combining a choice of energy (heat, electricity, and sound waves) and exercise therapy, depending on the purpose of treatment.
Contraindications and precautions for physiotherapy
Each physiotherapy modality cannot be used for individuals with certain implanted electronic devices, such as pacemakers, or for those with contraindicated conditions, diseases, or affected areas. In addition, there are physiotherapy modalities that are prohibited to be used in certain combinations. We will provide safe treatment under the specific direction of the physician.
Outdoor activity support
For social and daily life activities that involve outdoor mobility after discharge from the hospital, we support outdoor walking practice, use of public transportation, and shopping as part of rehabilitation.

Independent practice (home work)
To make the best use of time outside of rehabilitation, we also promote independent practice (home work) for patients. We will create a self-guided practice menu tailored to each patient's needs and encourage them to practice in their leisure time to achieve their rehabilitation goals earlier.